|
Calculation: (Total payments) divided by (total charges) minus (contracted amount and bad debt) plus (refunds). The result minus 100% shows how much revenue is lost due to underpayments, uncollectible bad debt, inaccurate adjustments, and posting errors. Regent RCM’s gold standard is greater than 97%.
 EvaluateQuestions?
AAFP members can ask a question at the Practice Management Help Desk.
In just six minutes, you can learn how to calculate your practice’s net adjusted collection rate. After watching this presentation, you will know how to:
The adjusted collection rate represents the percentage of reimbursement collected from the total amount allowed based on contractual agreements and other payments, i.e., what you collected versus what you could have/should have collected. This metric shows how much revenue is lost due to factors in the revenue cycle such as uncollectible bad debt, untimely filing, and other noncontractual adjustments.
Best Practice Tips
Calculating Adjusted Collection Rate
To calculate the adjusted collection rate, divide payments (net of credits) by charges (net of approved contractual agreements) for the selected time frame and multiply by 100.
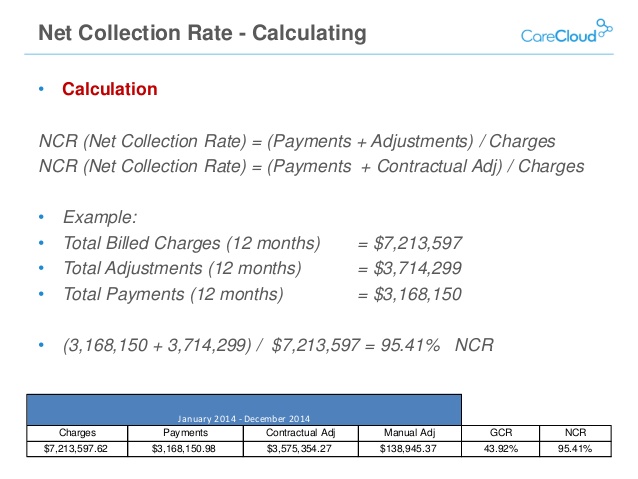 Sample Calculation
Other Considerations
Inappropriate write-offs.
One of the most common mistakes when posting payments is applying inappropriate adjustments to charges.
This page will be removed from your Favorites Links. Are you sure?
EvaluateQuestions?
AAFP members can ask a question at the Practice Management Help Desk.
This six-minute presentation quickly helps you learn how to calculate your practice’s denial rate. After watching this presentation, you will know how to:
The denial rate represents the percentage of claims denied by payers during a given period. This metric quantifies the effectiveness of your revenue cycle management processes. A low denial rate indicates cash flow is healthy, and fewer staff members are needed to maintain that cash flow.
Best Practice Tips
Calculating Denial Rate
To calculate your practice’s denial rate, add the total dollar amount of claims denied by payers within a given period and divide by the total dollar amount of claims submitted within the given period.
Sample Calculation
Other Considerations
Failure to identify mistakes prior to claim submission. Mistakes made during coding and charge entry can result in claims that are adjudicated and rejected by a payer. Establishing an internal process to identify and correct any mistakes prior to claim submission will decrease denial rates and produce a healthier cash flow.
The denial rate represents the percentage of claims denied by payers during a given period. This metric quantifies the effectiveness of your revenue cycle management processes. A low denial rate indicates cash flow is healthy, and fewer staff members are needed to maintain that cash flow.
This page will be removed from your Favorites Links. Are you sure?
 Comments are closed.
|
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
December 2022
Categories |
 RSS Feed
RSS Feed
